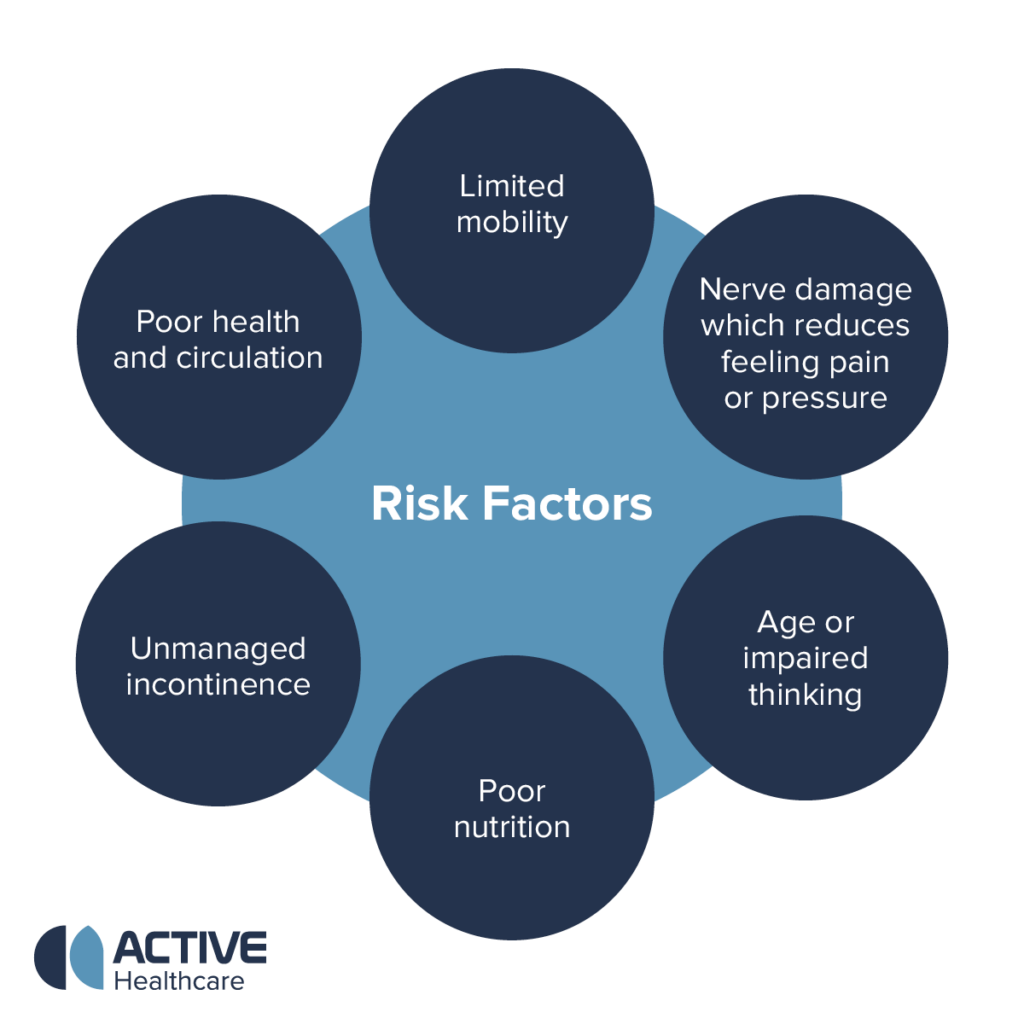
Healthcare-associated infections cost New Zealand $226 million in 2021. Skin or soft tissue infections contribute to the majority of these types of infections. We know that skin injuries occur when prolonged pressure and friction against the skin and leads to infections. As demonstrated in the above diagram, there are may risk factors that can impact pressure injuries and their probability. In this blog post, we will explore some common risk factors for pressure injuries and discuss the importance of using pressure care mattresses as a crucial first step in prevention.
Following our visual guide above, the below stages can help to analyse the risk factors of an individual:
Limited Mobility
Individuals with limited mobility, such as those who are bedridden, wheelchair-bound, or have difficulty changing positions, are particularly susceptible to pressure injuries. Immobility reduces the body’s ability to shift and relieve pressure points, increasing the risk of constant pressure on specific areas.
Nerve Damage
Nerve damage, whether due to underlying medical conditions or physical trauma, can diminish a person’s ability to sense discomfort or pain in certain body parts. Without proper sensory feedback, individuals may unknowingly subject themselves to continuous pressure, leading to the development of pressure injuries.
Age or Impaired Thinking
Advanced age or impaired cognitive function can contribute to a higher risk of pressure injuries. Elderly individuals or those with conditions like dementia may have difficulty recognizing and responding to discomfort or taking appropriate measures to alleviate pressure. Additionally, memory loss or confusion can hinder the ability to follow proper repositioning routines.
Poor Nutrition c
Proper nutrition plays a significant role in maintaining healthy skin and overall health. Malnutrition or inadequate intake of essential nutrients can weaken the skin’s integrity, making it more susceptible to damage. Inadequate hydration can also impair skin elasticity, further increasing the risk of pressure injuries.
Unmanaged Incontinence
Unmanaged incontinence, whether due to age, illness, or other factors, can significantly contribute to the development of pressure injuries. Constant exposure of the skin to moisture, as well as the presence of urine or feces, can cause skin breakdown, making it more vulnerable to pressure-related damage.
Poor Health and Circulation
Underlying health conditions, such as diabetes, cardiovascular diseases, or compromised circulation, can impair blood flow to tissues. Reduced blood supply diminishes the body’s ability to heal and repair damaged skin, increasing the risk of pressure injuries.
Prevention Strategies: Pressure Care Mattresses
One of the most effective steps in preventing pressure injuries is the use of pressure care mattresses. These specialized mattresses are designed to distribute pressure evenly across the body, reducing the concentration of pressure on vulnerable areas.
We recommend the following products as a guide, according to the pressure injury risk factors and category:
Category Four Injury:
Category Three Injury:
Category Two Injury:
Category One Injury:
If you are unsure, please give our team a call and we can walk you through prescribing the right pressure care mattress for your patient.
In recent years, there has been growing recognition of the importance of addressing pressure injuries as a public health issue. The NPIAP, EPUAP and Pan Pacific Pressure Injury Alliance (PPPIA) have worked in collaboration to develop a new pressure injury prevention and treatment clinical guideline. The intent of the collaboration is to advance international consensus in pressure injury prevention and treatment, and provide guidance and support for healthcare professionals and organizations working to prevent these injuries(1).
Despite these efforts, pressure injuries remain a significant concern in New Zealand and around the world. In addition to the human toll, the economic costs associated with these injuries underscore the need for continued investment in prevention and treatment efforts. By increasing awareness and implementing evidence-based strategies, our team can work with you towards reducing the incidence of pressure injuries and improving outcomes.. We are happy to prescribe the right pressure care solution for your patient and their environment.
References:
- European Pressure Ulcer Advisory Panel, National Pressure Injury Advisory Panel and Pan Pacific Pressure Injury Alliance. Prevention and Treatment of Pressure Ulcers/Injuries:
Clinical Practice Guideline. The international Guideline. Emily Haesler (Ed.). EPUAP/NPIAP/PPPIA: 2019
2. KPMG Pressure Injury Report 2016 (2015) The case for investment in: A quality improvement programme to reduce pressure injuries in New Zealand.
from https://www.hqsc.govt.nz/assets/Our-work/System-safety/Reducing-harm/Pressure-injury/Publications-resources/KPMG-pressure-injury-report-Jan-2016.pdf